Crisis & Mental Health Support
If you or someone you know is in crisis or struggling with chronic pain, please reach out:
- 988 Suicide & Crisis Lifeline (U.S.) — Call or text 988 | 988lifeline.org
- Crisis Text Line (U.S., U.K., Canada, Ireland) — Text HOME to 741741 | crisistextline.org
- Samaritans (U.K. & Ireland) — Call 116 123 (free, 24/7) | samaritans.org
- Lifeline Australia — Call 13 11 14 | lifeline.org.au
- International Association for Suicide Prevention — Find a crisis centre
- Endometriosis UK Helpline — Call 0808 808 2227 | endometriosis-uk.org
Myth 1: “It’s just a bad period”
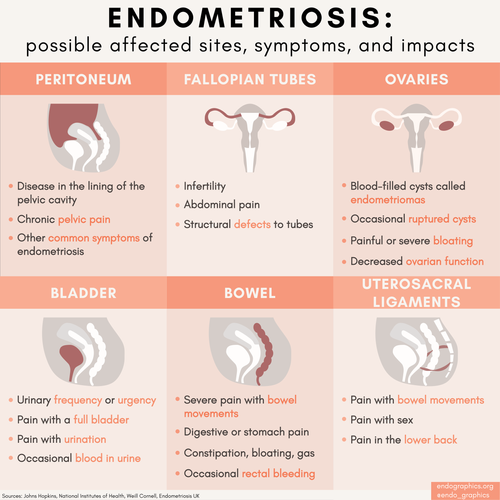
Fact: Endometriosis is a systemic, inflammatory disease where tissue similar to the uterine lining grows outside the uterus — on the bowel, bladder, diaphragm, and other organs. It causes chronic pain, organ damage, and infertility. It is not a variant of normal menstruation.
“Endometriosis is a disease characterized by the presence of endometrium-like tissue outside the uterus, which induces a chronic, inflammatory reaction.” — World Health Organization (WHO)
Myth 2: “Pregnancy cures endometriosis”
Fact: Pregnancy does not cure endometriosis. Some people experience temporary symptom relief during pregnancy due to hormonal changes, but the disease persists and symptoms typically return afterward. Endometriosis can also make it harder to become pregnant in the first place.
“Pregnancy does not cure endometriosis… symptoms may recur after pregnancy.” — American College of Obstetricians and Gynecologists (ACOG)
Myth 3: “Hysterectomy cures endometriosis”
Fact: Hysterectomy removes the uterus, but endometriosis grows outside the uterus. If lesions on the bowel, bladder, or other sites are not excised, pain and disease progression can continue after hysterectomy. Hysterectomy may help with adenomyosis specifically but is not a guaranteed cure for endometriosis.
“Hysterectomy is not a cure for endometriosis… disease can persist or recur if lesions outside the uterus are not removed.” — Endometriosis Foundation of America (EndoFound)
Myth 4: “Endometriosis only affects the reproductive system”
Fact: Endometriosis has been found on the bowel, bladder, diaphragm, lungs, liver, sciatic nerve, and even the brain. It is associated with increased cardiovascular risk, autoimmune conditions, and a 31% increased risk of early mortality.
“Endometriosis is associated with increased risks of several chronic diseases… including cardiovascular disease, autoimmune conditions, and certain cancers.” — BMJ 2024
Myth 5: “You’re too young to have endometriosis”
Fact: Endometriosis has been diagnosed in adolescents as young as 10–11 years old. Dismissing young patients’ pain leads to the current average diagnostic delay of 7–10 years.
“Endometriosis in adolescents is a significant clinical entity… early diagnosis and treatment can prevent progression of disease.” — PMC: Endometriosis in Adolescents
Myth 6: “Birth control cures endometriosis”
Fact: Hormonal birth control can suppress symptoms by reducing menstruation, but it does not eliminate endometriosis lesions. The disease can progress silently while symptoms are masked. Stopping hormonal treatment typically leads to symptom return.
“Hormonal treatments suppress the disease but do not eradicate it… the recurrence rate after discontinuation is high.” — ESHRE Guideline on Endometriosis
Myth 7: “It’s just a low pain tolerance”
Fact: People with endometriosis experience central sensitization — their nervous system amplifies pain signals due to years of chronic inflammation. Research shows measurable changes in how the brain and spinal cord process pain. This is neurological, not psychological.
“Central sensitization contributes to the chronic pain experienced by women with endometriosis… manifesting as hyperalgesia and allodynia.” — PMC: Central Sensitization in Endometriosis
Myth 8: “Endometriosis is caused by lifestyle choices”
Fact: Endometriosis is not caused by diet, exercise habits, stress, or any lifestyle choice. The exact cause is unknown, but research points to genetic factors, immune dysfunction, and possibly stem cell involvement. No one is to blame for having this disease.
“The cause of endometriosis is unknown… there is no known way to prevent it.” — World Health Organization (WHO)